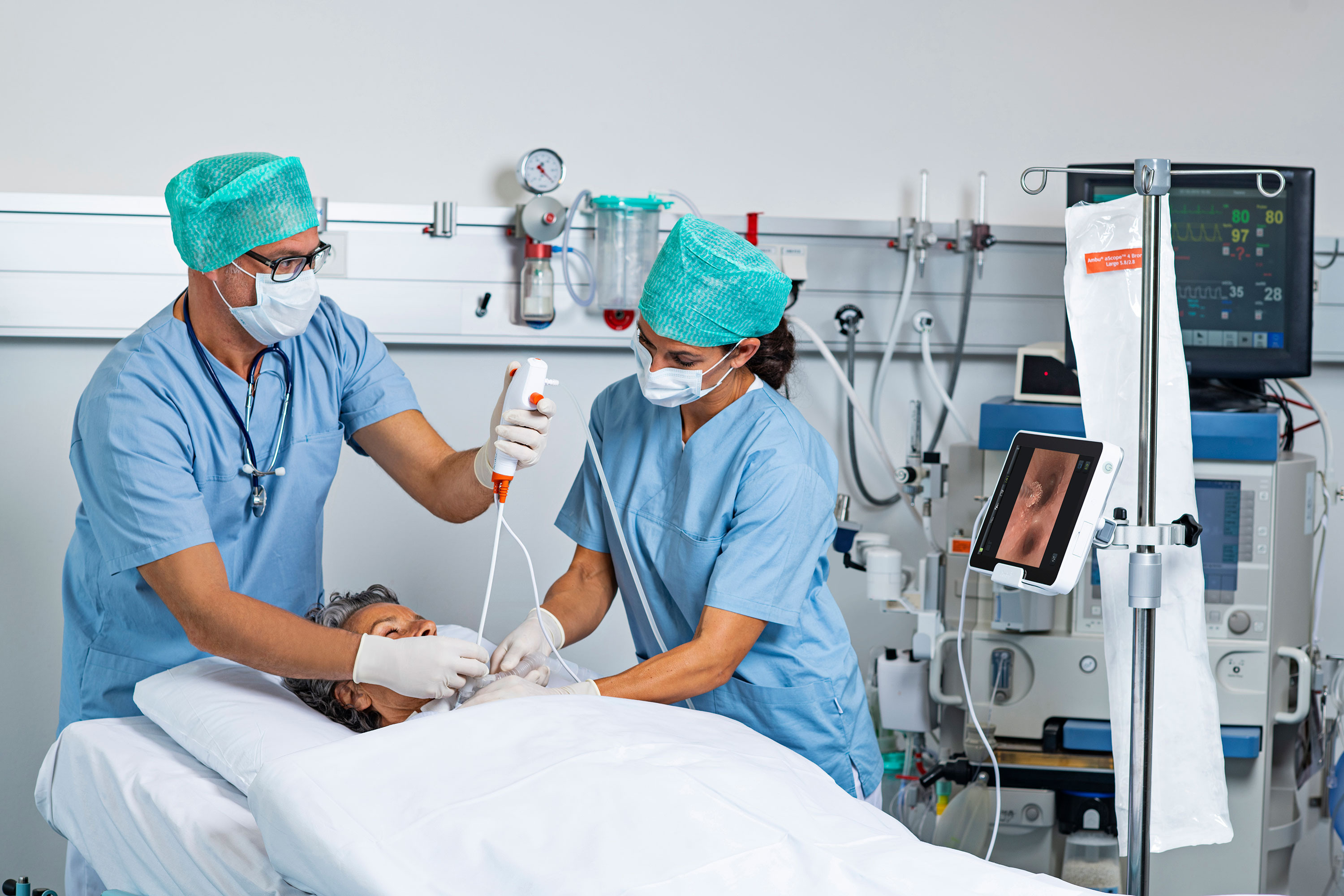
One manual wash cycle prior to high-level disinfection (HLD) may be sufficient in adequately disinfecting duodenoscopes utilizing disposable tips.
That’s according to evidence presented by researchers from Duke University at ACG 2022 last October, who found that one manual wash did not lead to significantly more bacteria than two cycles prior to HLD.
The authors write that duodenoscopes with disposable components “appear to have decreased bacterial contamination” but don’t eliminate it entirely. That was the takeaway of another poster also presented by the same researchers from Duke at the annual meeting.
“Our data provide impetus for larger studies of abbreviated HLD protocols and the development of technologies that expediate the HLD process,” the poster concludes.
Last year, the U.S. Food and Drug Administration updated a safety communication recommending that facilities transition to innovative duodenoscope designs due to concerns about reprocessing and patient cross-contamination. Those recommendations include utilizing fully single-use duodenoscopes or models with disposable components.
“The best solution to reducing the risk of disease transmission by duodenoscopes is through innovative device designs that make reprocessing easier, more effective, or unnecessary,” the communication says.
Recently updated standards and guidelines additionally call for sterilization rather than HLD for certain “high-risk” endoscopes, including duodenoscopes.
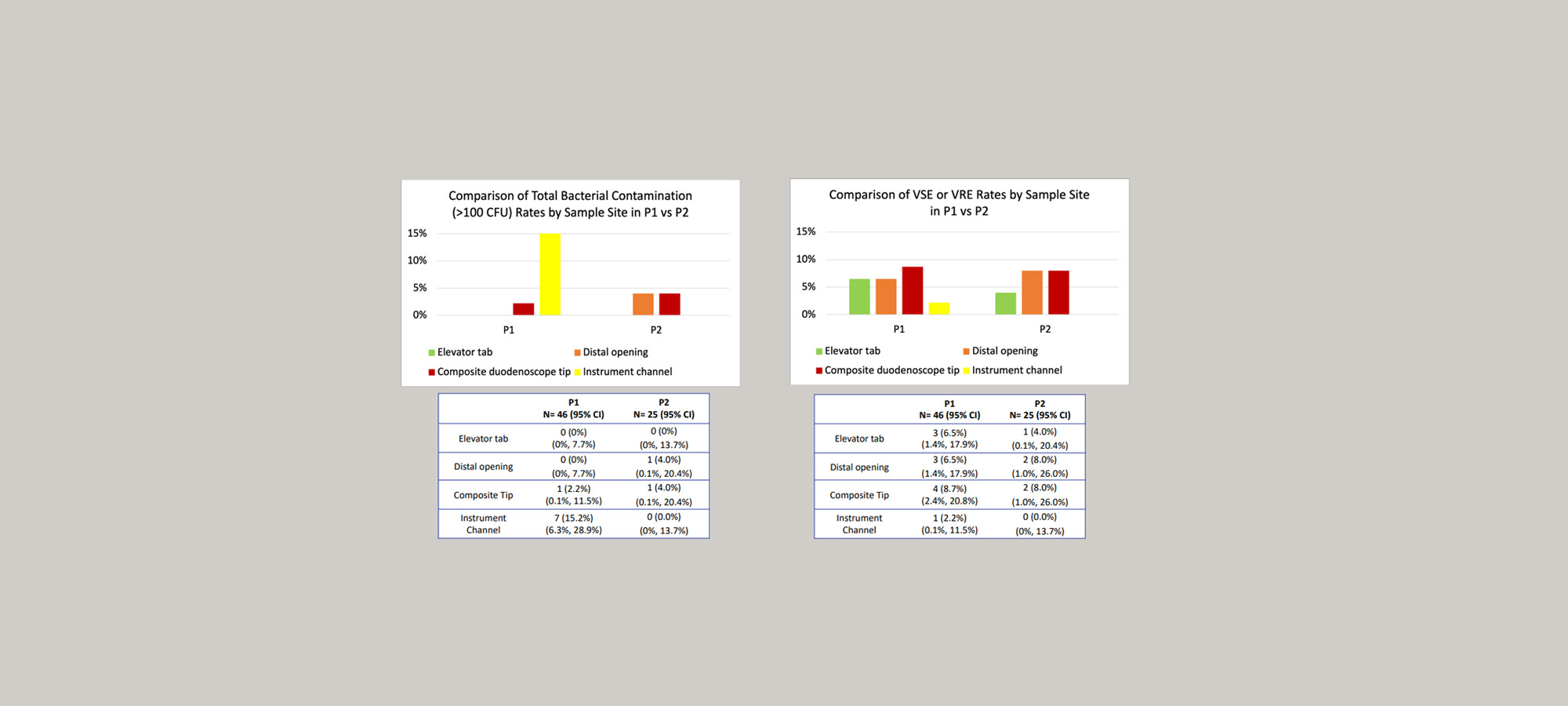
The Duke researchers conducted the study in two phases. The first assessed efficacy of abbreviated HLD protocols with one manual wash cycle and the second one reviewing standard HLD protocols. Phase one included 46 duodenoscopes sampled at four sites apiece, with eight sites having greater than 100 culture forming units (CFU) of raw growth and 11 sites with either Vancomycin sensitive or resistant Enterococcus (VSE/VRE).
Phase two included 25 duodenoscopes also sampled at four sites each. Two out of 100 had raw growth of greater than 100 CFU and five grew VRE.