ENTs can expect to be key players in the care of people suffering long-term effects as a result of contracting COVID-19.
That’s according to a report in ENTtoday, which notes the lingering symptoms from the virus that causes COVID-19 can include continued loss of taste and smell, shortness of breath, headaches, fatigue, mental fogginess, cough, chest pain, joint pain and other symptoms.
Those symptoms can persist for months and make ear, nose and throat specialists “uniquely positioned” to help these patients on their road back from SARS-CoV-2.
In some cases, the virus has caused lasting heart or lung damage. But, perhaps more frustrating are the many patients who have persistent symptoms, yet show no evidence of organ damage.
A recently published meta-analysis of 27 studies found loss of smell in 48.47 percent of the pooled global sample of COVID-19 patients, according to ENTtoday. Comparable data for loss of taste was 41.47 percent, while about 35 percent of patients experienced both loss of smell and taste.
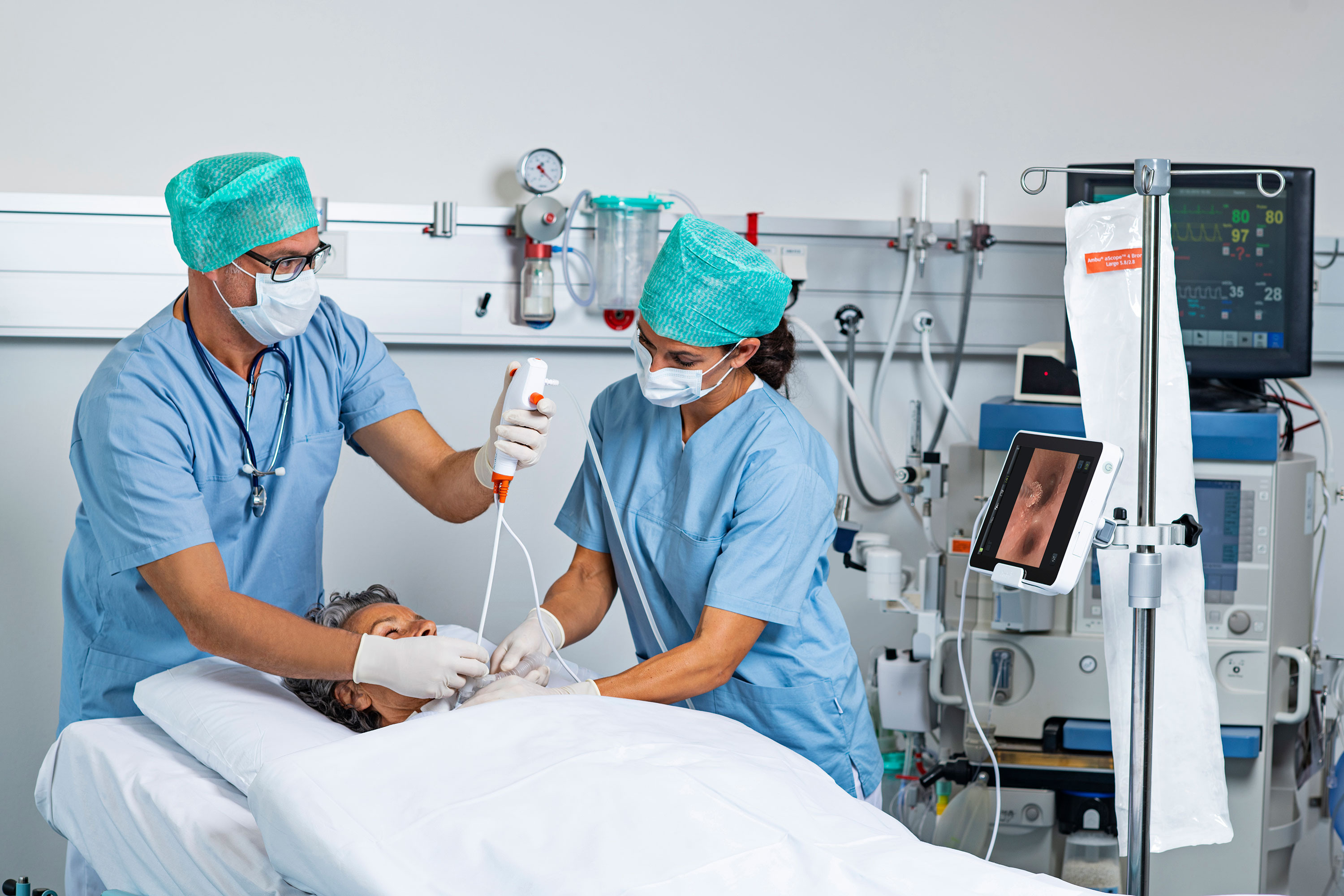
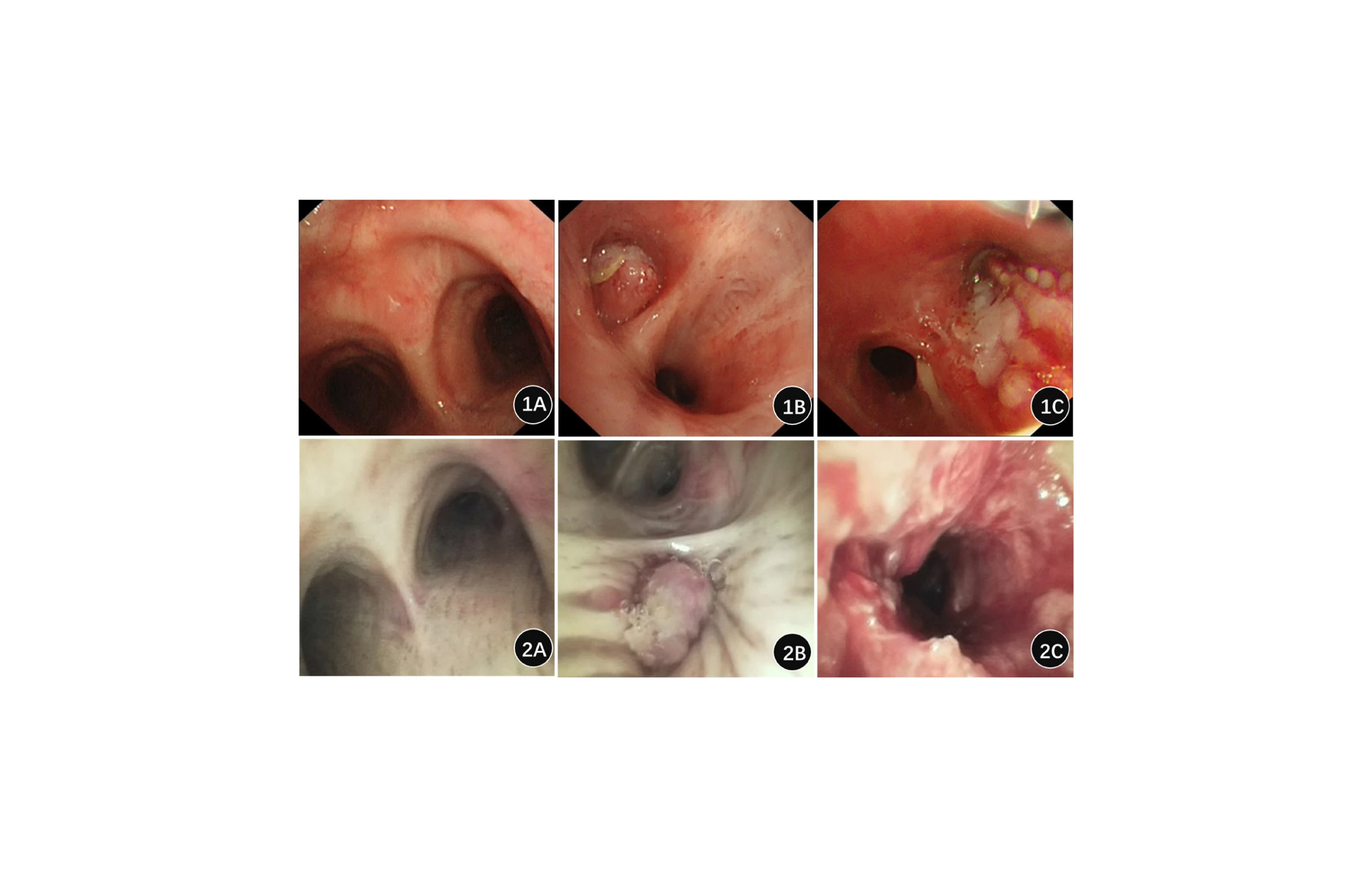
Patients who suffer from continued shortness of breath after COVID-19 but have normal chest X-rays and lung CTs may have a treatable condition caused by inflammation of the vagus nerve, detectable by laryngoscopy. That nerve, which stretches from the neck to the abdomen, carries signals back and forth between the brain and the digestive system and organs.
The key question to ask a patient with these symptoms is whether the shortness of breath or cough wakes them up at night, says Dr. Jonathan Aviv. If not, the cause is almost always the result of a problem with the vagus nerve, he tells ENTtoday.
If larygngoscopy shows vocal folds not moving in normal synch with a patient’s breathing — for instance, closing more than 50 percent when they should be opening — respiratory retraining and a low-acid diet may ease the symptoms. Respiratory retraining involves increased resistance breathing exercises, typically administered by a speech-language pathologist and can even be administered virtually.
Aviv and his colleagues documented success with all the patients they treated this way, according to a study published in the International Journal of Pulmonary & Respiratory Sciences.
In July, the European Laryngological Society recommended that “every patient with a history of a COVID-19-related ICU stay should be followed after discharge by an otolaryngologist or other airway specialist to proactively diagnose early complications at the level of the larynx and trachea.”
However, any patients who continue to experience COVID-related symptoms should consider an ENT consult.
“Otolaryngologists will have to educate the public (as well as their colleagues in other disciplines) about the essential role they can play in the diagnosis and management of post-COVID-19 complications,” ENTtoday reports.