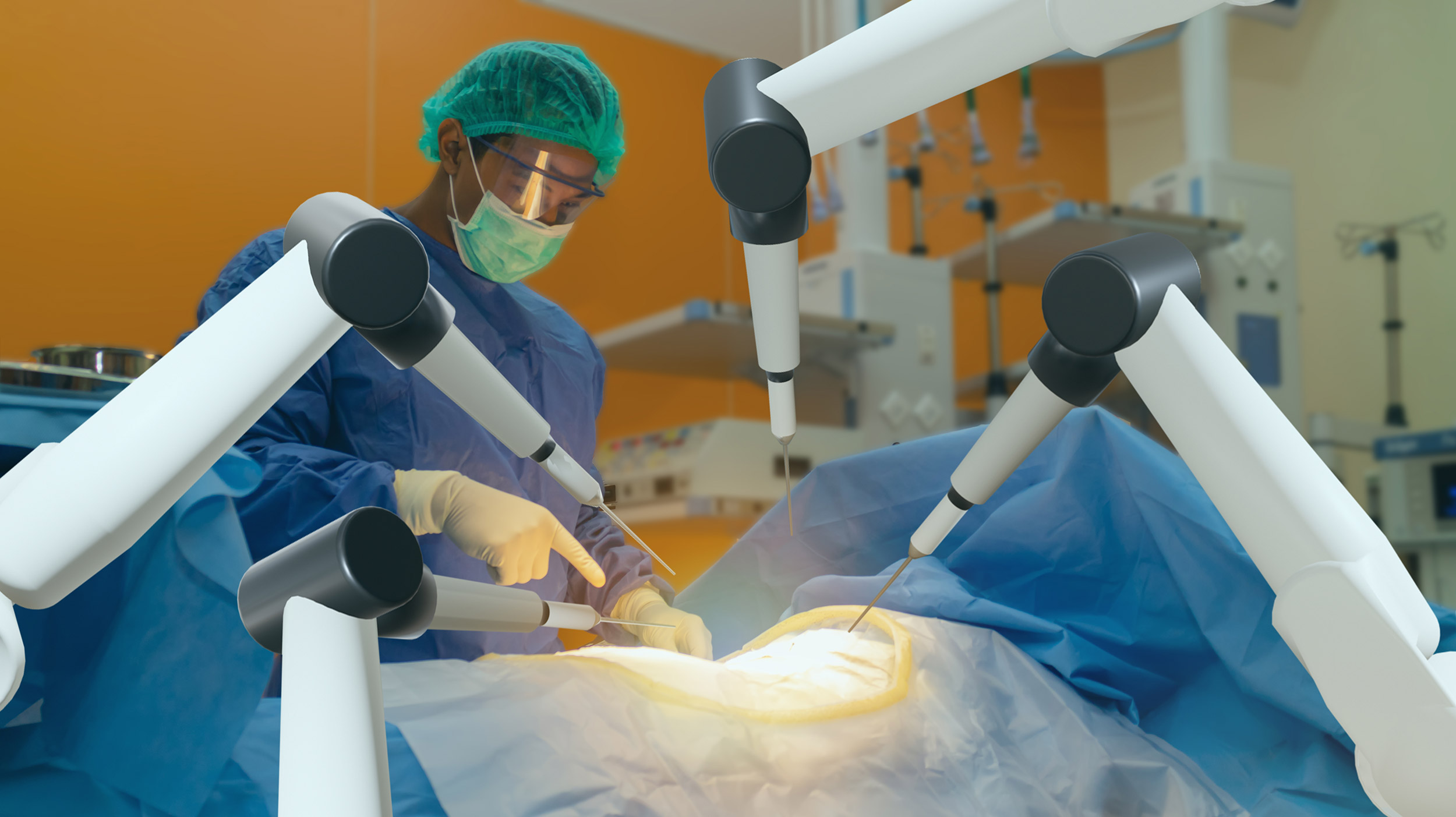
This year’s American Urology Association (AUA) annual meeting in New Orleans placed a spotlight on the latest cutting-edge technology. Numerous sessions focused on robotic technology and its usefulness to the urology community.
Some of the highlights included a new robotic ureteroscope with laser technology promising a more comprehensive range of motion. There was also a discussion on emerging robotic surgical systems in urology, and a debate to determine which medical robotic-assisted prostatectomy device was superior.
Second-Generation Ureteroscopes
A single-use ureteroscope featuring robotic technology, laser automation, and a video game-like joystick that is more comfortable to operate was featured during a “state-of-the-art lecture” on new technology that’s in store.
“A robotic ureteroscope will be able to make movements we currently can’t make with our existing ureteroscopes,” said presenter Dr. Ben H. Chew.
Second-generation ureteroscopes also offer enhanced resolution, imaging, and contrast, Chew added.
The advantages of robotic ureteroscopes include the use of ergonomic human machine interfaces (HMI). They include hardware or software through which an operator interacts with a controller, allowing for smoother and more precise tool movement.
Competition Coming to Robotic Surgical Systems
The world of robotic surgery is gradually shifting as several new platforms have been authorized or are in the approval pipeline.
During an AUA panel entitled, “Laparoscopic Robotic Surgical Systems-Emerging Systems in Urology Use,” urologists discussed some state-of-the-art robots currently in use.
Until recently, robotic surgical systems were mostly used for laparoscopy procedures.
“There is growth in new types of procedural-specific robotics such as flexible and rigid endoscopic robotics as well,” said moderator Dr. Duke Herrell, a urologist and director of the minimally-invasive urologic surgery and robotics program at Vanderbilt Health.
At least two manufacturers are developing flexible robots that will enhance future generations of flexible ureteroscopes, Herrell added.
Some pulmonologists are using robotic bronchoscopy to examine tiny lung masses for biopsies that are too difficult to reach with a traditional bronchoscope.
Battle of The Bots
Which is the superior product, a single-port or multi-port robotic prostatectomy device? This was a question that participants debated in a “Battle of the Bots” discussion.
Dr. Jihad Kauok, a urologist at the Cleveland Clinic, and Dr. Jeffery A. Cadeddu, a urologist at the University of Texas Southwestern Medical Center, debated the pros and cons of single-port versus multi-port robotic prostatectomy.
A multi-port robotic prostatectomy requires a surgeon to make six incisions inside the prostate, while a single-port system requires only one.
Multi-port robotic prostatectomy is the gold standard for the surgical management of localized prostate cancer because there are fewer complications, less blood loss, and shorter hospital stays, Cadeddu said.
It’s not whether the single-port robotic platform is a better option, Dr. Kauok began by saying, but how doctors can utilize the platform to better serve specific patient populations to improve outcomes.
Single-port systems offer a customized approach and don’t require patients to use opioids, as well as improved ergonomics and the ability to choose a different approach for surgeons.
Single-port robotic systems also enable physicians to see more patients, Kaouk added. Both doctors agreed there is room for both — in the end, the only thing that matters is the best outcome for a patient.


