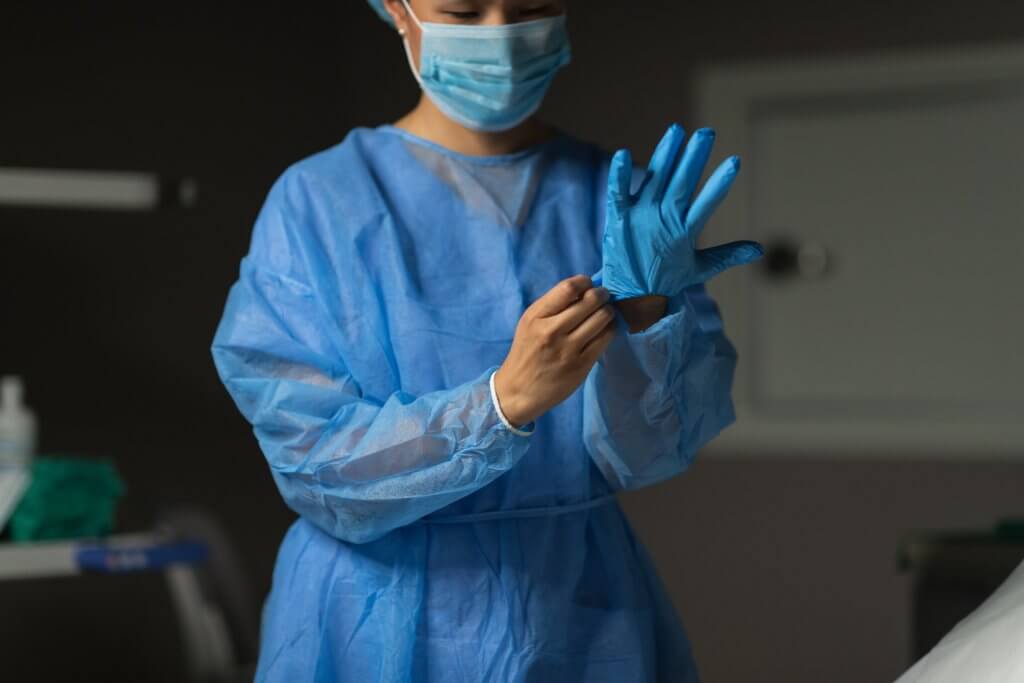
Personal protective equipment (PPE) is vital to keep endoscope reprocessing staffers safe. Used incorrectly, however, and PPE can undo the important work of endoscope disinfection.
That’s why adequate surveillance of endoscope reprocessing should include checks on proper PPE usage. Because flexible endoscopes are exposed to mucous membranes and nonintact skin, they may carry harmful contaminants after a procedure. PPE is essential to protecting reprocessing personnel from those human contaminants as well as the chemicals needed to remove them.
Endoscope reprocessing involves a complicated series of between 50 and 100 steps depending on the device instructions for use (IFUs) and society guidelines adopted by the institution. Individual endoscope reprocessing steps may vary slightly by the type of endoscope and manufacturer.
Among the 50 to 100 steps needed to reprocess flexible endoscopes are several PPE changes to protect the integrity of the cleaning process. Handling a freshly disinfected duodenoscope coming out of an automated endoscope reprocessor (AER) without fresh gloves, for example, can re-contaminate a scope.
Without PPE, pathogens could be transmitted from patients to reprocessing personnel, or healthcare workers could be exposed to dangerous disinfectants.
Reprocessing guidelines from three key organizations – the American National Standards Institute and Association for the Advancement of Medical Instrumentation (ANSI/AAMI) and the Association for perioperative Registered Nurses (AORN) – instruct reprocessing technicians to don scrubs, head covers, shoe covers, impermeable gowns, fluid-resistant face masks, face shields or goggles, and gloves.
The gowns, masks, eyewear, and gloves are essential to keep reprocessing technicians safe from hazardous materials, blood, and disinfectants, which can irritate and harm the eyes, throat and skin.
Reprocessing personnel are also instructed to:
Gloves, worn as a protection against infectious agents and bodily fluids, can also transmit pathogens from one surface to another. A 2016 study that analyzed cross-contamination rates between gloves and hospital surfaces found that contaminated gloves increase the risk of cross-transmission of healthcare-associated infections among healthcare workers and the environment.
The American National Standards Institute and Association for the Advancement of Medical Instrumentation (ANSI/AAMI) reprocessing guidelines outline nine instances in which gloves should be changed during endoscope reprocessing.
“Don fresh PPE, including gloves and skin and eye protection” – that’s the direction given at the start of each of the following reprocessing steps:
The guidelines also state that gloves should be changed between loading and unloading an endoscope into and from an automated endoscope reprocessor (AER).
All these PPE changes are vital to the integrity of the cleaning process, according to the ECRI Institute.
“Endoscopes that have been cleaned but not yet high-level disinfected are still contaminated with viable microbes; thus gloves used to handle an endoscope at that stage must not be used to remove the scope from the reprocessing machine,” according to the ECRI Institute’s 2019 report on the top 10 health technology hazards.
The report also notes that removing an endoscope from an AER after high-level disinfection with unclean gloves compromises the scope’s cleanliness.
A 2018 review of the three hospital reprocessing suites found that technicians did not change gloves between handling a soiled scope and after one had been disinfected. The study also revealed technicians would reuse towels to wipe down endoscopes, rather than changing towels for every endoscope.


