Infection transmission during bronchoscopy has not historically been well tracked or documented, which means the true risk of infection has been difficult to quantify.
A new study, however, has found bronchoscopy-induced infection risk to be 2.8 percent based on a review of 3,120 procedures that resulted in 86 infections. The study, which was conducted in London in November 2019, also confirmed previous findings that single-use bronchoscopes are cost-effective compared with reusable bronchoscopes used in flexible bronchoscopy procedures, tracheal intubation and double-lumen tube position.
“A systematic review and cost effectiveness analysis of reusable vs. single-use flexible bronchoscopes” by J.M. Mouritsen, L. Ehlers, J. Kovaleva, I. Ahmad and K. El-Boghdadly combined a comprehensive analysis of literature with a micro-costing study of flexible bronchoscope use at the Guy’s and St. Thomas’s NHS Foundation Trust Department of Anaesthesia in London. Two of the authors have previously consulted for Ambu. Ambu did not fund this study.
Single-use bronchoscopes do not require reprocessing or routine maintenance and “there are currently no reported cases of cross-contamination using single-use flexible bronchoscopes, which is why the risk is expected to be 0 percent.”
Approximately 500,000 bronchoscopic procedures are performed in the United States annually. The perceived infection risk has always been low, but many experts also say that the true rate of infection has likely been underreported.
The 2.8 percent infection risk was based on a review of 16 studies from six different countries. When pulling out the eight studies that were conducted in the U.S., the infection rate was 3.6 percent.
Tracheal intubation and double-lumen tube position were among the procedures included in the study. Costs for these procedures using reusable flexible bronchoscopes were compared to the cost of the Ambu aScope 4 Bronchoscope and aView monitor.
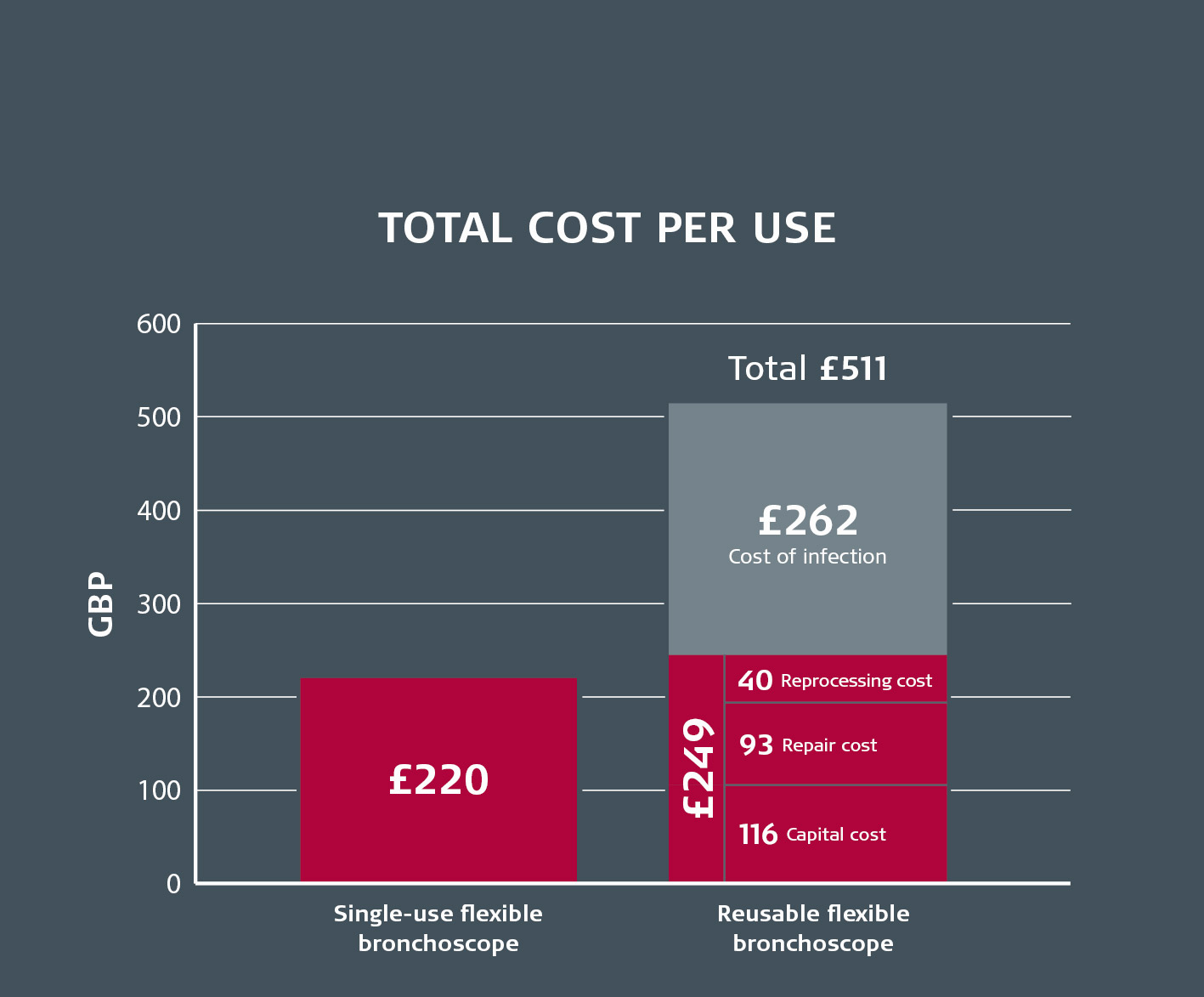
The cost analysis and determination per procedure included bronchoscope repairs, service agreements, and reprocessing labor at the British medical center. Treatment costs related to post-bronchoscopic infection were also included in the analysis.
Missing from the study were cases in which patients may have contracted a pulmonary infection after a bronchoscopy while under general anesthesia. The authors cite an incidence rate of 23 percent for postoperative pulmonary complications—including pneumonia and sepsis—for patients having general anesthesia. The infection incidence rate is higher among patients undergoing head and neck surgery, the authors note. However, these cases were not included in the study because no data exists that directly correlates bronchoscope-induced infection in these patients. Infections in these cases are often determined to be “multifactorial,” according to the study.
Using an Ambu aScope 4 bronchoscope, the study concluded, costs an average of 12 percent less per procedure, before infection risk was considered, as compared to a reusable bronchoscope. When factoring in costs for treating infection, single-use flexible bronchoscopes cost up to 57 percent less per procedure.
More information about the study can be found at ambuusa.com/ascope-4-broncho-guys.