There is no reprocessing method that has been demonstrated to completely eliminate the risk of cross-contamination from duodenoscopes. Researchers at Indiana University Health, however, sought to find out if one method of reprocessing duodenoscopes may be superior to another, with the goal to better protect patients from device-related infection during endoscopic retrograde cholangiopancreatography (ERCP).
Guidelines for reprocessing duodenoscopes between uses are lengthy and vary by manufacturer. Double (or repeat) high-level disinfection (DHLD) and liquid chemical sterilization (LCS) were both tested during the study, which spanned from October 2017 until September 2018 and Indiana University researchers found no discernable difference between the quality of cleaning and subsequent surveillance cultures of the scopes when comparing DHLD and LCS.
Dr. Mark Gromski, an assistant professor at the Indiana University School of Medicine, presented the findings of the study at the 2019 American College of Gastroenterology meeting, held in San Antonio, Texas. Gromski stressed that both methods—DHLD and LCS—required adequate manual precleaning at the point of use in order to be effective.
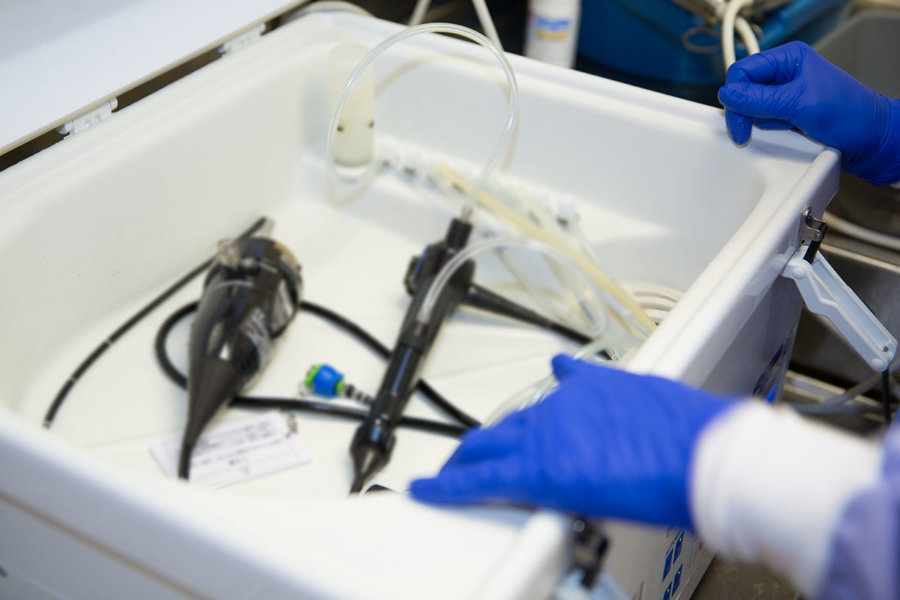
Duodenoscopes feature an elevator mechanism and long flexible tubes that make them particularly difficult to clean and disinfect after use. Numerous infection outbreaks have been traced back to reprocessed duodenoscopes that were still harboring infectious organisms, trapped in broken parts, on the distal ends, or protected by biofilm.
Duodenoscopes in the DHLD group were manually cleaned and then went through two cycles in an automated endoscope reprocessor (AER). Duodenoscopes in the LCS group were similarly cleaned prior to the sterilization.
Of the 453 surveillance cultures from the duodenoscopes that underwent DHLD, 1.8 percent were positive for organisms after reprocessing. The LCS group—425 cultures—saw a positive culture rate of 2.1 percent. Only two cultures in each of the groups were “high concern” organisms.
There were no positive cultures for multidrug-resistant organisms in the study. Since MDROs are increasingly difficult to treat, protecting against device-related infection of resistant organisms is of high concern. There were no known transmission of organisms to patients during the study period.
Gromski concluded that the two methods were equal in effectiveness in reprocessing duodenoscopes. Both systems could be easily implemented, Gromski said. In the study, the average reprocessing time for duodenoscopes when practicing DHLD was 98 minutes, verses 55 minutes for LCS.
Gromski’s research also found the recurring costs (not including capital costs) under each method to be similar: $10.30 per duodenoscope when performing DHLD and $8 per duodenoscope when using LCS during reprocessing, according to preliminary analysis of unpublished data.
One important factor when it comes to costs, Gromski said, is that Indiana University Health is a high-volume center for ERCPs. More than 27,000 procedures are performed there annually. Research shows that procedural volume can impact on physicians' success rate in ERCP procedures, as the procedures are highly complex. Similarly, Gromski said, so is the reprocessing protocol for duodenoscopes.
The reprocessing procedures for duodenoscopes are long and complicated, and without regular practice, those tasked with reprocessing them may fall out of regular practice, impacting the effectiveness. The opposite may also be true in high-volume centers, where the demand for a fast turnaround time between procedures may put intense pressure on cleaning staff to move through reprocessing procedures with an eye on efficiency.
In August 2019, the New York Times published a story on the infection risks associated with reprocessed duodenoscopes used during ERCP procedures. This article was closely followed by an op-ed in the same newspaper, written by several ERCP specialists, that outlined the benefits of an ERCP. The benefits to having the procedure far outweigh any potential infectious risks, the doctors wrote.
The debate around potential infections caused by contaminated duodenoscopes stretches back to 2013, when the Centers for Disease Control and Prevention first alerted the U.S. Food and Drug Administration to the potential for device-related cross contamination from these flexible endoscopes.
For years, the agency has been searching for ways to make these vital, life-saving procedures even safer for patients. Potential solutions that have been discussed by the agency include making certain parts of a duodenoscope disposable.
As a matter of protocol, Gromski said, he and other physicians walk through the risks of the ERCP procedure, which includes potential risk of infection. Over the years, the medical center has made numerous changes to internal reprocessing and infection control protocols to try and minimize the risk of infection transmission.
As a medical center with the largest volume of ERCP procedures nationwide, Gromski said it was important for Indiana University to conduct this research and attempt to lead the way in mitigating some of the risks posed by duodenoscopes.
“We view it as our obligation to do the best we can,” Gromski said.


