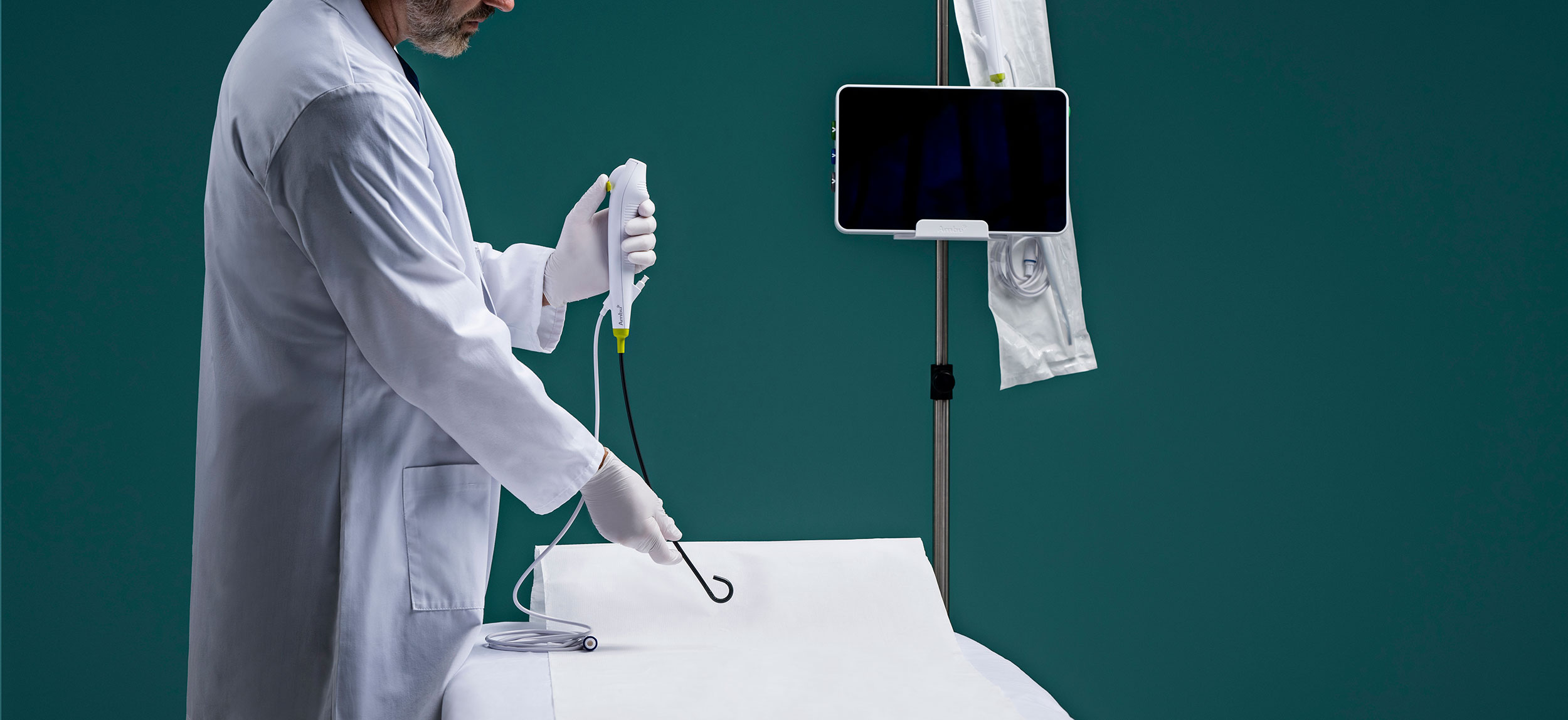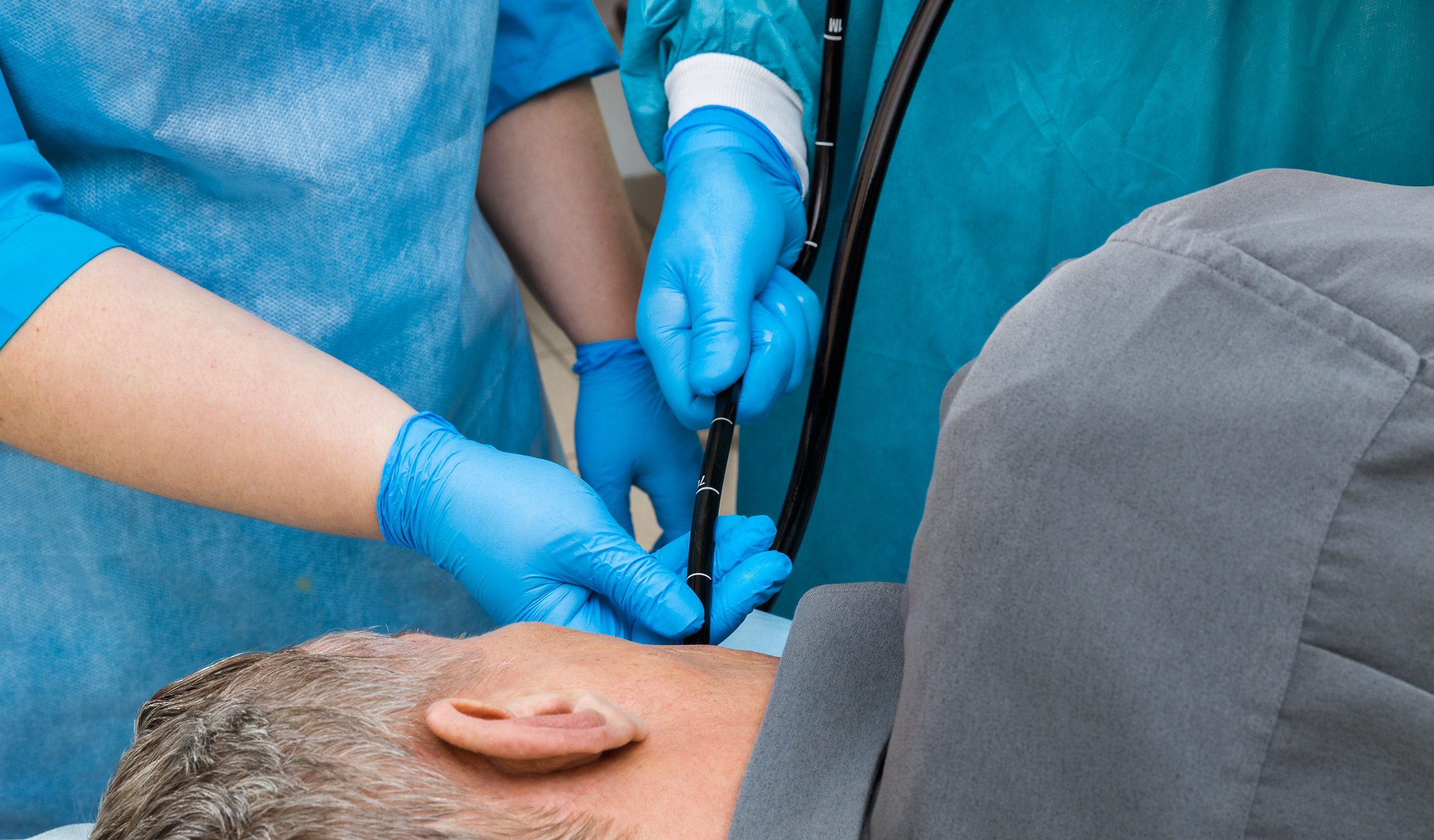
Endoscopic retrograde cholangiopancreatography (ERCP) is arguably the most difficult advanced endoscopic procedure.
But the clinical challenges fall to more than the GI endoscopist maneuvering a duodenoscope and accessories to diagnose or palliatively treat problems in the pancreatic and bile ducts.
Registered nurses serving in the GI suite need to understand the indications, complications, and workings of ERCP, according to Nancy Schlossberg, program director of Digestive Health Services at John Muir Health. Only then can they provide the best care before, during and after a procedure.
 In recognition of National Nurses Week (May 6-12), Schlossberg spoke with Single-Use Endoscopy about the vital role nurses play in successful ERCP patient care and infection prevention. The 2021 theme for International Nurses Day (May 12) is “Nurses: A Voice to Lead.”
In recognition of National Nurses Week (May 6-12), Schlossberg spoke with Single-Use Endoscopy about the vital role nurses play in successful ERCP patient care and infection prevention. The 2021 theme for International Nurses Day (May 12) is “Nurses: A Voice to Lead.”
In addition, Schlossberg — who has more than 40 years of clinical and industry experience — shared how new FDA-approved single-use duodenoscopes can assist nurses in providing a safe environment for patients in the GI suite.
SUE: What are the main roles nurses play in the GI suite during advanced endoscopic procedures like ERCP?
Schlossberg: Endoscopy is about everybody on the team.
Many nurses today are comfortable assisting in the technician role, as well as assuming the role of the circulating nurse. Each role is important in ensuring the safety, efficiency, cost-effectiveness, and promotion of optimal patient outcomes by recognizing and responding appropriately to changes in the patient's health status.
While on the topic, whether your team is all RNs or a mix of RNs and technicians, the importance of hands-on, competency-based team training facilitates a more cohesive team and efficient workflow leading to more positive patient outcomes.
SUE: Since ERCP is such a complex procedure and poses several unique risks to patients, what can nurses do to provide the best care in these cases?
Schlossberg: GI nurses who understand the indications, complications, and dynamics of an ERCP are in the best position to provide pre-, intra-, and post-procedure education and expectations to the patients, families, significant others, and caregivers.
For example, because pancreatitis is the most common complication of ERCP that may develop in response to mechanical manipulation of the papilla or injection of contrast during the procedure, pre-procedure patient teaching would include post-procedure symptoms of pancreatitis and sepsis (e.g., chills, low grade fever, pain, vomiting and tachycardia) requiring the patient to immediately notify their physician.
SUE: When it comes to patient safety and preventing infection, what is the nurse’s role in the GI suite?
Schlossberg: Ultimately, GI nurses serve as patient advocate and act as a resource for others.
Nowhere is this more important than in the role of infection prevention, especially when it comes to cleaning and processing duodenoscopes. Duodenoscopes have been associated with cases of infection despite confirmation that the users were following proper manufacturer cleaning and disinfection or sterilization instructions. Manufacturer’s instructions for use, governmental and regulatory agency, as well as professional society guidelines are ever evolving.
I especially encourage GI nurse managers to take part in the SGNA Infection Prevention Champion program, which appoints a champion who takes responsibility to become familiar with and communicate practice guidelines and industry practice changes to their peers.
SUE: The potential for device-related infection in the GI suite has come under increased scrutiny in recent years, especially given U.S. FDA investigations into cross-contamination from duodenoscopes. How do nurses contribute specifically to preventing duodenoscope-associated infection?
Schlossberg: Nurses working in units that perform ERCP, or any other endoscopic procedure for that matter, have a good understanding of cross-contamination. In the procedure room, staff demonstrate proper hand hygiene, use of PPEs, movement of instruments and personnel from dirty to clean and, very importantly, demonstrate competence in pre-cleaning endoscopes following the removal of the scope from the patient. Nurses also ensure proper storage of endoscopes to prevent cross-contamination.
However, the various types of personnel who clean and reprocess endoscopes may have different educational and competency needs than the staff member working in the actual reprocessing area. The staff member who performs only bedside pre-cleaning will demonstrate competencies specific to that crucial task that must be performed in a timely manner to avoid formation of biofilm, ensure patient safety, and allow the device to remain in proper working order.
SUE: Given media reports around duodenoscope-associated infection, do you find patients are concerned prior to ERCP procedures?
Schlossberg: Patients have expressed concern; however, physicians have done a good job discussing the risks and benefits associated with the procedure. Over the past year, COVID-19 has caused more patients to raise concerns or delay endoscopic procedures.
SUE: How do recent FDA recommendations for an industry switch to partially or fully disposable duodenoscopes affect patient care?
Schlossberg: This is an evolving question. Recent literature compares economic, environmental and infection-related risks and benefits associated with single-use scopes. Reprocessing protocols and changes in duodenoscope design such as detachable distal tips and elevators continue to evolve. However, we continue to hear reports of duodenoscope-transmitted infections even after duodenoscopes have undergone reprocessing according to manufacturer’s instructions.
Each endoscopy setting should assemble a multidisciplinary team (endoscopy physician and nursing leadership, infection prevention, risk management, endoscope reprocessing personnel, facility leadership, materials management, etc.) to develop an evidence-based approach to determine what is best for their facility as newer technologies such as single-use duodenoscopes continue to evolve. The endoscopy nursing, physician leadership and reprocessing personnel are key stakeholders as end users and reprocessors, respectively, of the newer technologies. Expenses related to performing ERCP will likely increase given new reprocessing and scope technologies.
However, safety first! All involved need to appreciate the cost and risk of a single infection tied to improper reprocessing at their institution!
SUE: Can you pinpoint specific ways single-use duodenoscopes may benefit patients?
Schlossberg: Endoscopy nurses are very familiar with delaying and canceling procedures because a scope is delayed in reprocessing or out for repair with no loaners available. How much physician, patient and staff frustration does this engender? How does this impact a patient’s length of stay? Single-use duodenoscopes, which require no reprocessing or repair, potentially streamline workflow.
In addition, a single-use scope, that requires no reprocessing, eliminates the possibility of reprocessing related human error that plays a large part in ERCP infections.