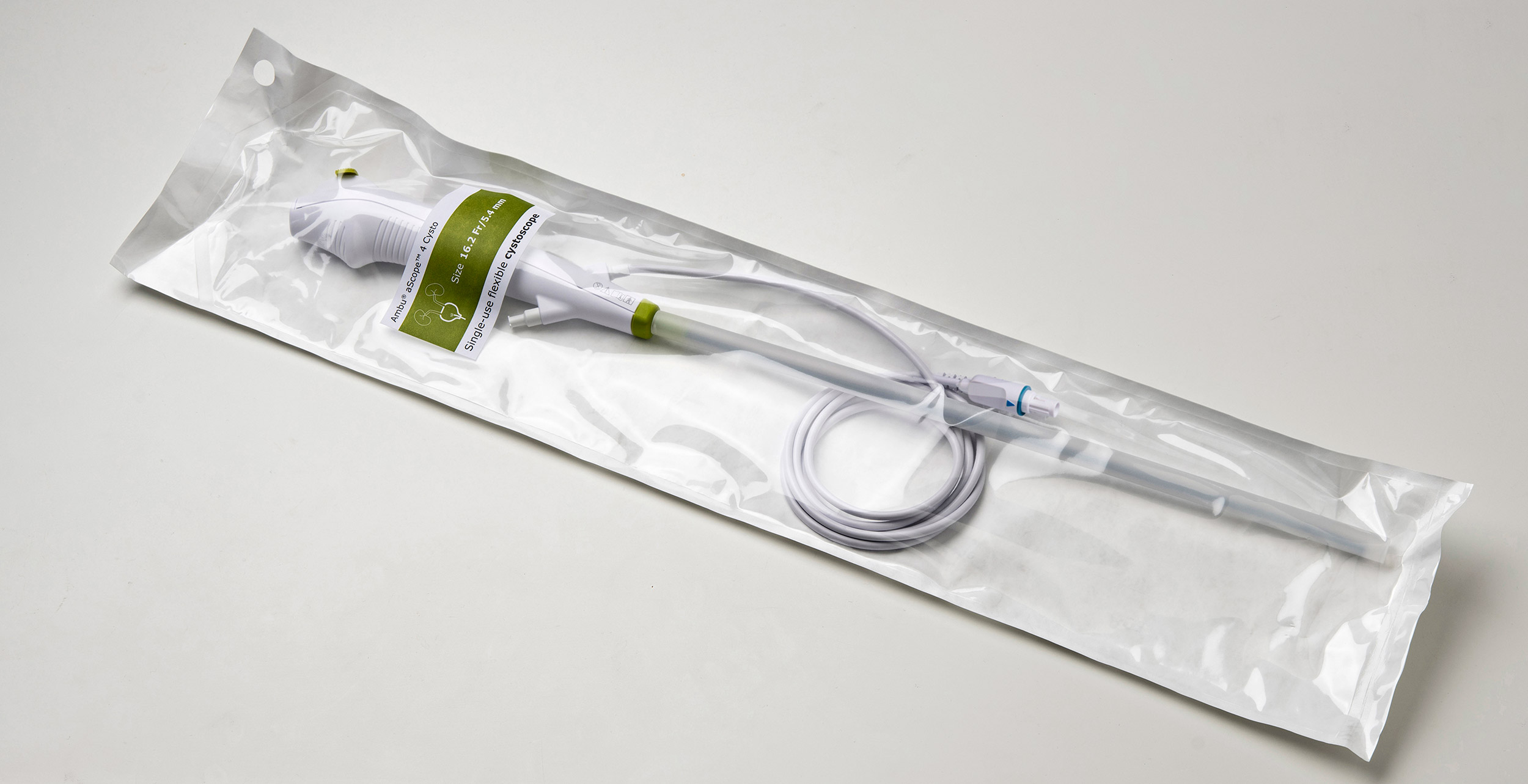
Surveyed individuals indicated they would be significantly more willing to transition to single-use cystoscopes in clinical practice if at least one of the following four factors were true:
The authors of a May Research and Reports in Urology study investigated worldwide market readiness of single-use flexible cystoscopes through a survey of urologists and procurement managers (PMs) in France, Germany, Italy, Spain, the United Kingdom, Japan, and the United States from March to May 2020. The survey received 415 responses from 343 urologists and 72 PMs.
Three study authors disclosed that they are employees of Ambu A/S, a manufacturer of single-use cystoscopes, and two authors are consultants for the company.
The authors calculated the conversion rate by asking respondents to anticipate which procedures they would consider using a single-use cystoscope for. On average, respondents would consider using a single-use scope for 44.5 percent of all procedures.
Survey participants had not previously used a single-use cystoscope at the time of the study. Their assessment assessment was based only on descriptions of a single-use cystoscope’s benefits and features.
Of the 415 respondents, 221 indicated concern about infections from contaminated reusable cystoscopes. While rare, infection outbreaks have been traced to contaminated reusable cystoscopes.
The U.S. Food and Drug Administration recently announced an investigation into numerous medical device reports describing patient infections and other possible contamination issues and the potential link to urological endoscopes. The urologists and PMs that participated in this survey answered questions about infection control one year prior to the FDA announcement.
In addition to infection concerns, single-use cystoscopes offer greater cost transparency for numerous reasons, including “incalculable hidden costs associated with failed cleaning cycles” and potential contamination, the authors write.
“Compared to a reusable setup, single-use offers a more streamlined process with no hidden costs associated with labor time, reprocessing equipment, and repairs, making the per procedure cost more transparent in a single-use setup,” the authors write.
Respondents from Italy had the highest conversion rate at 57.5 percent. Japanese respondents reported the lowest at 23.7 percent. The age of oldest cystoscope in use among respondents from Japan was lower than any other country. The average age of oldest reusable scope in use across all respondents was 6.2 years.
The authors write that many reusable cystoscopes are designed to have a seven-year shelf life and “performance associated with the risk of cumulative wear and tear should be considered” when using a scope beyond that age. This may explain 276 respondents experiencing lost image quality or a lack of appropriate maneuverability of reusable scopes.
Single-use ureteroscopes, another type of urological endoscope, are widely adopted and have been found to provide many advantages over reusable ones. However, single-use cystoscopes have only recently begun to gain awareness, the authors write.