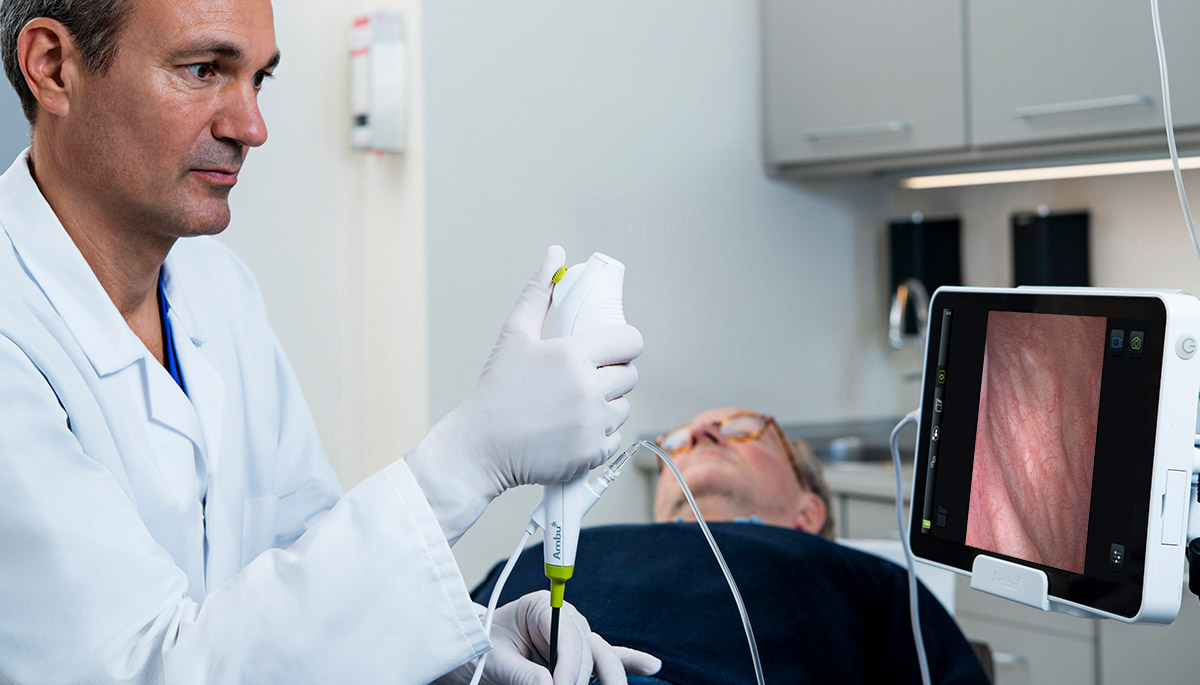
The per-procedure cost of flexible cystoscopy varies by institution and the cost-effectiveness of single-use cystoscopes could largely rely on procedural volume.
That's according to a May 2021 study in Urology, which explores factors such as capital equipment costs, labor, and supply costs, as well as the number of procedures performed each year, to see how they impact the price of cystoscopy. The study is authored by Alexander P. Kenigsberg, Samuel Gold, Lorie Grant, and Yair Lotan.
“It may become more cost-effective for relatively less-common in-hospital bedside cystoscopies to be performed using disposable scopes,” the authors conclude. “Furthermore, the portability may allow the disposable scope to be used in a room that may not have space for a traditional tower with monitor. Likewise, clinics without sufficient staff or resources to resterilize scopes readily might be able to provide more access to cystoscopy if they incorporate use of disposable scopes.”
Doctors from the department of urology at the University of Texas Southwestern Medical Center in Dallas performed 3,739 flexible cystoscopies in 2019. The department has nine reusable cystoscopes in circulation, so each was used in an average of 415 procedures that year.
Per-procedure costs consist of capital, maintenance, reprocessing, labor, and disposable supplies.
A separate analysis of labor workflow was conducted to calculate labor costs. Only labor for the procedure itself and the price of disposable procedural supplies were included in calculating per-procedure costs with single-use cystoscopes.
In the study, entitled “The Economics of Cystoscopy: A Microcost Analysis,” researchers from the Dallas center calculated the cost of cystoscopy utilizing a reusable scope sterilized with an AER to be $161 per procedure at their facility.
When high-level disinfection (HLD) was the reprocessing method, the cost dropped to $133 per procedure. The projected cost for a cystoscopy performed with an Ambu single-use cystoscope was calculated to be $222.
The key factor, however, is the minimum number of procedures performed.
The authors determined that for a reusable cystoscope to be cheaper than a single-use alternative, it would need to be used for 196 or more cystoscopy procedures per year when reprocessed with an AER. If using HLD, a reusable scope becomes cost effective when used in at least 145 procedures per year. Based on factors such as capital investments and maintenance contracts, single-use cystoscopes become the cost-effective option if their reusable counterparts do not perform those minimum number of procedures.
The cost of the cystoscope itself came out to $21 per case for reusable and $175 per case for single-use.
AER usage added $2.80 per case for reusables. The machine’s maintenance contract was $7.20 per cystoscopy and maintenance contracts for reusable scopes were $22.70 per procedure.
Per-procedure cost increases as procedure volume decreases. Reimbursement varies with many factors, but commercial insurance provided more than Medicare.
A 2020 study in the Journal of Endourology found single-use cystoscopes to be a cost-effective alternative to reusable scopes, with the standard version requiring an extraordinarily high number of annual uses to be the economical choice. Other studies have found single-use endoscopes in other clinical areas may also be a cost-effective solution.
And there's the issue of infections related to reprocessed urological endoscopes: The U.S. Food and Drug Administration announced in April 2020 that it's investigating numerous medical device reports describing patient infections and other contamination issues possibly associated with reprocessed cystoscopes, ureteroscopes, and cystourethroscopes.