November is Bladder Health Month, and urinary incontinence has been a focal point of this year’s outreach.
Urinary incontinence is more common among women, according to the Urology Care Foundation — affecting an estimated 30 to 50 percent of women — and that means gynecologists are often tasked with diagnosis and treatment.
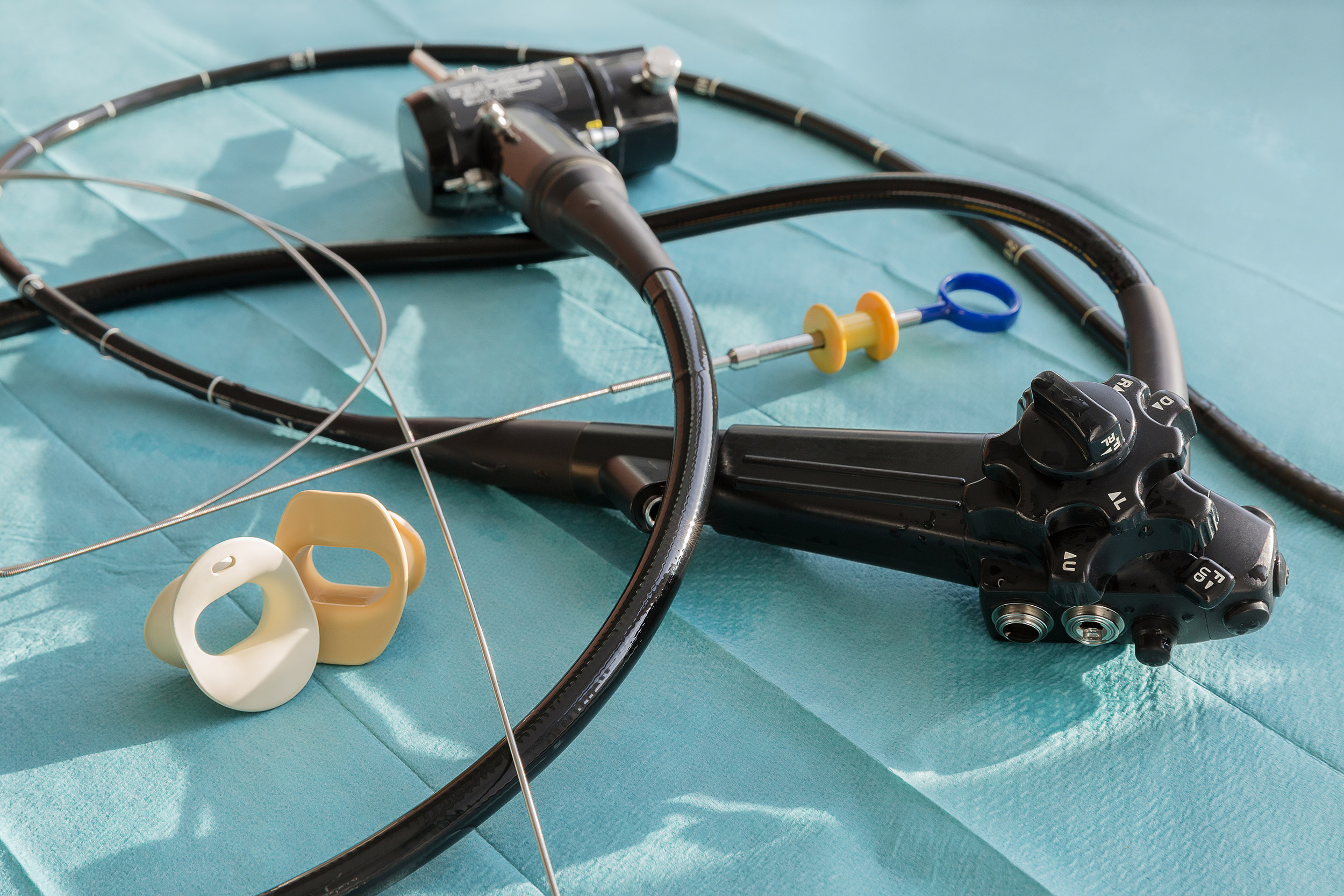
When assessing the bladder, it is common for physicians to turn to cystoscopy, a minimally invasive procedure that sends a long, flexible tube with a camera on the end, up the urethra to gain a view of the bladder. A recent study found gynecologists may benefit from increased exposure to cystoscopy in residency, to increase their comfort level with the procedure and boost competencies.
More than 50 OB-GYN residents were surveyed as a part of the study. Most (84 percent) felt comfortable and satisfied with their cystoscopy volume and training. Almost half of the respondents had completed more than 30 cystoscopies in a training setting.
The Accreditation Council for Graduate Medical Education (ACGME) requires gynecology residents to complete 10 cystoscopies for full competency. Through their qualitative cross-sectional review of survey results, researchers found at least double that number may be beneficial. Half of the responding residents believed at least 20 cystoscopies should be required to obtain competency in the skill.
“Given the move toward universal cystoscopy, consideration should be made to increasing the current requirement,” the study, published in the American Journal of Obstetrics and Gynecology, concluded.
Bladder Health Month serves as a valuable time to spread awareness of the ways everyone can improve bladder health, according to the Urology Care Foundation. Even urinary incontinence, which affects an estimated 25 million people, can often be treated with simple lifestyle changes.